This information HAS errors and is made available
WITHOUT ANY WARRANTY OF ANY KIND and without even the
implied warranty of MERCHANTABILITY or FITNESS FOR A
PARTICULAR PURPOSE. It is not permissible to be read by
anyone who has ever met a lawyer or attorney. Use is confined to
Engineers with more than 370 course hours of engineering.
If you see an error contact:
+1(785) 841 3089
inform@xtronics.com
The blood clots get paved over with new intima - what is leftover from the clot is now called plaque. The same process causes restenosis which plugs up stents. The layers of old clots end up narrowing the artery - and is in fact the key symptom of CAD. The cholesterol in plaque comes from the membranes of red blood cells. (Red blood cells are made up of 40% lipids). This perfectly explains the cholesterol crystals in plaque.
The Cholesterol theory of CAD is dead - the initma is a tight
junction - LDL can not go through it. Much work was done to
find a transport - they failed - several attempts were never
published. You cant form cholesterol crystals from cholesterol
esters - it HAS to come from the red-blood cell membranes.
Sickle-cell
Smoking
Air pollution
High BG (Thins the protective glycocalyx)
High blood pressure
Lead (Pb)
Other heavy metals
Lack of sunshine (low Vit-D? Or NO or other?)
Stress
High homocycsteine
High Lp(a)
Erectile dysfunction (low NO?)
Restricted sodium (quadruple rate)
VEGFI
Proton pump inhibitors (via NO) (doubles risk)
Note - the above have a commonality - they all mess with the
endothelial health - increase tears which lead to clots..
Low vit-C
Viagra class drugs - 3-fold reduction of risk(YMMV)
Magnesium
Potassium
ACE inhibitors - (increase NO)
Mechanisms
of lead-induced hypertension and cardiovascular disease
Rose Sick individuals vs populations
Lp(a) is just LDL that delivers APO(a) to form a blood clot. It
is genetically related to
plasminogen - it forms clots that the body has trouble
removing.
The LDL found in plaque isn't LDL - it is Lp(a)
We know that oxLDL is a much better predictor of events than any score calculated from lipid panels. (see Tests_for_Preventative_Heart_Health- see Oxidized_LDL_assay). Interventions based on lowering of oxLDL rather than the narrow focus on LDL appears to be the best bet. Normal LDL does not seem to be a risk other than it can become oxLDL. OxLDL is related to inflammation.
possible? Molecular
mechanism of glutathione-mediated protection from oxidized
low-density lipoprotein-induced cell injury in human
macrophages: Role of glutathione reductase and glutaredoxin
Inhibition
of Glutathione Production Induces Macrophage CD36 Expression and
Enhances Cellular-oxidized Low Density Lipoprotein (oxLDL)
Uptake
L-Carnitine
Rosemary
Anthocyanins Pomegranate Quercetin Lycopene cocoa (non Dutched) Iodine
Olive-oil polypheols
CoQ10 ?
taurine (might protect from oxLDL) Luteolin might protect Differential inhibition of oxidized LDL-induced apoptosis in human endothelial cells treated with different flavonoids ginseng - might protect L-theanine (green tea) might protect?
:*
Tryptophan might increase oxLDL http://dx.doi.org/10.1016/0021-9150(91)90254-Z Dietary oxChol - see next section!High-quality fish oil has a more favourable effect than oxidised fish oil on intermediate-density lipoprotein and LDL subclasses: a randomised controlled trial
poor quality fishoil
One bit that the public is not aware of is that between 1960 and today, the amount of PUFA's (Poly Unsaturated Fats) in our diets has increased 5x - this is a result of breeding frost resistant strains - this corn, soy and wheat accounts for most of the carbon in our food supply. The problem is too much PUFA is not good for us. It causes a lot of people to get fat and produces systemic inflammation - which leads to things like CAD, depression, joint pain, and a list of other health problems.
I can look at my old high-school pictures (1970s) and we were not over weight. If you look at high-school kids today, you will see that more than half are now over weight. This is likely a result of the increased PUFA's and sugar in the diet ( the combination is REALLY bad).
Excess PUFAs interfere with insulin-blood-glucose regulation.
Fish oils block some of the bad effects of PUFA - but not all -
best to avoid all vegetable oil based foods - corn fed chicken and
any chips, anything deep-fat-fried, salad dressings - are big
sources . there is beef, fish etc. Eat fish - not fish oil.
Could be that just eating real foods that contain them is the
best idea.
I think there is definite a red flag here - might explain the confusion with satFATS - satFats foods will often be refrigerated for some period - the longer the more oxy-CHOL. Particularly bad foods are powdered eggs, powdered milk - (dried whey protein ?) - these are found in all sorts of box food.. avoid those center isles.
...the quantity of oxidized lipids in their serum lipoproteins increased 16-fold and were significantly greater than in controls.
...in humans dietary oxidized lipids are absorbed by the small intestine, incorporated into chylomicrons, and appear in the bloodstream...
I think oxidized Cholesterol is probably connected to small Ldl - I don't understand this part yet.
oxidized lipids.. Sounds like modern beef is full of them - wish there was a study on grass-fed?
Looks like time is the critical factor - faster cooking is better.
Powdered eggs? I think not.
This may be a good reason to modify a lowcarb diet to avoid oxidized cholesterol and may explain some of the inconsistencies of the earlier studies.
When I was on my failed lowfat diet for years I used a lot of "non-fat powdered milk" - did I do myself harm? (Thank you AHA)
I have these crazy questions that I keep thinking about - What changes have we made to our foods that have increased CAD?
What if freezing meat before cooking changes lipids in some way? Perhaps we are a lot better eating freshly butchered meats?
I'm thinking that OCP(Oxidized Cholesterol Products)(sometimes COPs) may help guide an optimal diet plan. Meanwhile, it does appear that dietary sources of OCP increase atherosclerosis. I've identified 3 sources so far: powered milk, powdered eggs and beef. The powdered products are found in processed box foods - again pointing in the same direction. One study claimed that cholesterol in beef was almost 100% oxidized. (Again I'm wondering if it is really the beef or it is in fact that the modern industrial marbling cattle diet that has us not researching real beef, but sick beef in particular.) How I would like to see an NMR lipid profile and OCP numbers on grass fed vs fattened beef (even to look at 10 cattle).
I was asked: "If you eat low carb you become insulin resistant?"
Yes! - hopefully. Any diet that works - has to create insulin resistance. Insulin resistance is what lets fat leave adipose tissue(fat cells). ( You can also get into ketosis by any calorie restriction - normal people are in ketosis when they wake up - and this state includes some insulin resistance.)
If you are insulin sensitive and/or have a high insulin level - fat accumulates in adipose tissue. Only when you are insulin resistant and have lower insulin can fat leave these cells.
From wikipedia: There is a constant flux of FFA (Free Fatty Acids) entering and leaving adipose tissue. The net direction of this flux is controlled by insulin and leptin—if insulin is elevated, then there is a net inward flux of FFA, and only when insulin is low can FFA leave adipose tissue. Insulin secretion is stimulated by high blood sugar, which results from consuming carbohydrates.
The adipose insulin sensitivity is controlled by the F:N ratio that Petro talks about:
Remember:
LPL move fat in to fat cells. HSL
moves fat out of fat cells.
insulin is known to activate LPL
in adipocytes
HSL is inhibited by insulin.
So here is the take home - there is nothing wrong with being insulin resistant - IF BG and thus insulin is low. Two ways to get there - starvation diet or low-carb.
This is a simplification - other bits are involved - leptin, ASP
are also involved and there are effects of the autonomic nervous
system as well. Remember that man does not know his biology
completely - so likely there are bits we are missing.Also insulin
apparently has the opposite effect on muscle tissue - as it should
see Effects of
insulin and exercise on muscle lipoprotein lipase activity in
man and its relation to insulin action.
Could be that the bacterial shower from eating food starts up an immune response that triggers systemic inflammation. Improving the gut barrier may be important.
The 11 Critical Conclusions from Good Calories, Bad Calories:
My father was an OB Gyn back when he lived in Wisconsin and used a 'glucose tolerance test' to check pregnant women for gestational diabetes. I remember him telling me that fasting blood sugar can miss diabetes - resulting in major problems for pregnant women. My father once had a Dr. Edgar Gordon as his endocrinology professor (UW) - the doctor who's 1963 JAMA diet article that inspired Dr. Atkins to write his variation. (My fasting sugar has always been fine and I've never had a 'glucose tolerance test' at a doctors office. In dealing with my reluctant doctor, I just ordered a case glucose and bought a cheap meter at Wall-mart - (total cost of $30 - less than a single lab fee!)).
See http://en.wikipedia.org/wiki/Glucose_tolerance_test
Because I had a whole case of glucola, I went ahead and tested my wife and daughter and found my wife had IGT(Impaired Glucose Tolerance) that our doctors fasting test missed. My wife has modified her diet (wish I could say the same for my daughter).
Why don't they do the 'glucose tolerance test'? Is it is too much of a hassle to have them come back in 2 hours?
When I was younger, I didn't think twice about eating sugar. Then I read some things that Dr Arthur Robinson Dr. Robinson (who was once a partner with Linus Pauling) wrote back in the late 90's and I decided to stop drinking any sugar drinks.
Today, I would not bother with the GTT - no one should be eating sugar - I just test my BG 1.5 to 2 hours after a meal - if it is over 110 I look at what and how much I ate and adjust my diet.
I was wondering if fructose might be better than glucose (it was recommended for diabetics as a substitute for sugar) and did some more digging and reading and started wondering about HFCS and finally wrote Dr Robinson. He kindly wrote back telling me about an experiment he did on astronaut diet. They wanted a diet that produced no feces in space so they just consumed pure amino acids and pure sugars and some pure lipids. Everything worked out rather well, but the population complained of some boredom, so they replaced the glucose with fructose as a test. The result was high triglycerides. He also told me that fructose has a separate metabolic pathway compared to sugar.
We now know that fructose is a toxin:
Next paper pretty much settles any doubt:
Further reading over the years has convinced me that high blood sugars cause an increase in AGE(Advanced Glycation End-products). These plaques are involved in macular degeneration, Alzheimer disease, kidney disease, arthritis, and of course CAD. One other bit of information is that fructose is 10 times more likely to form AGE than glucose. I can imagine that even a slightly higher exposure to fructose (like that in HFCS) over a life time could lead to an increase in disease. Not all HFCS is the same - most is 55% fructose but there are some that are 60 to 65% fructose. The fructose in HFCS is not a disaccharides (as sucrose) and thus the fructose is circulated through the entire body before hitting the liver. Honey, often tauted as a health food, is pretty much a natural HFCS Honey, often erroneously tauted as a health food that it is NOT:
* 38.5% Fructose * 31.0% Glucose * 1.0% Sucrose (metabolizes to 50:50 glucose and fructose) * 9.0% (maltose (di - glucose), melezitose (a a nonreducing trisaccharide sugar))
It is also important to note that because fructose has a separate metabolic pathway compared to sugar that path way can become 'backed up' and I don't know that anyone is measuring blood-fructose levels that I know of (why not?). I have been told that the carbohydrate lobby has covertly and successfully blocked studies on the effects of HFCS.
Taubes book confirmed many of the things I found out by exhaustive Google scholar searches. One of that take home points is that our bodies will increase adipose tissue(fat tissue) to an amount that might be able to protect us from high blood sugars. If I want to lose weight - I need to reduce my insulin . level. I don't think there is any other way - and that means limiting carbohydrates.
Not very useful - it is the area under the curve - time times the amount above 110 blood sugar that apparently counts. Being somewhat high for half a day is probably just as bad as being quite high for an hour. If one eats complex carbs then BG and insulin will be up for many hours and if ones insulin is up one CANNOT LOSE WEIGHT.
GI diets fool people into poor choices - Carbs should be reduced to keep postprandial sugars below 110 (use of an accurate meter is a must - most are not good enough). Don't fall for the low GI diet - it continues the carbohydrate addiction.
The high glycemic index dose will spike insulin and spike blood sugars for a relatively short time. Insulin will rise causing the body to store fat. High insulin levels are know to stimulate appetite (in fact insulin is sometimes given to anorexics to help get them to eat). Do the short but very high blood sugars cause major AGE damage?
If the same 100G of glucose come bound in fiber and slowly absorbed - my body is exposed to slightly higher blood glucose levels for a long period of time. Slight insulin increases - that may prevent weight loss are experienced for a long time - perhaps preventing any release of triglycerides form adipose tissue and preventing weight loss?
I don't think there is a clear answer if Glycemic Index is useful - it may be that the form of the carbohydrates is more important? Might maltose vs galactose vs sucrose vs mono-saccharides as the form of carbohydrate be more important than glycemic index? What we need is some research to clear this up - and some research on the effects of the different di and mono saccharides. I'm not one to encourage government regulation, yet I think it is clear that if cigarettes need a warning label - so do sugar foods.
According to:
Hcy-thiolactone is detoxified by Hcy-thiolactonase/paraoxonase present in a subset of high-density lipoprotein particles in humans.
(should we be taking calcium?)
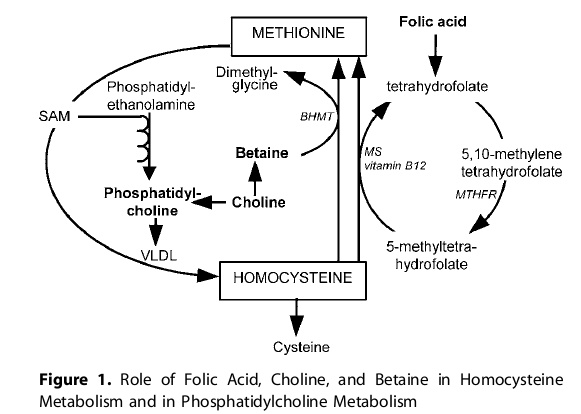
With that as a back ground - it appears that the methylation of
homocystein happens with folic acid with the B12 enzyme.
Polyenylphosphatidylcholine -> choline -> betane uses the
BHMT(Betaine-Homocysteine Methyltransferase enzyme). So the
question is: Pumping which system, BHMT or B12 Is it possible that
taking B vitamins and folic acid might do more harm than good?
Estrogen will lower LDL, high fiber, Alirocumab, Welchol,
Colesevelam, ezetimibe, Gemfibrozil, Niacin, repatha, PUFAs,
Fenofibric acid, mycophenolate mofetil, Alirocumab - many other
interventions..
They don't lower mortality.. They don't work - the cholesterol
theory is thus dis-proven?
| Top Page | wiki Index |